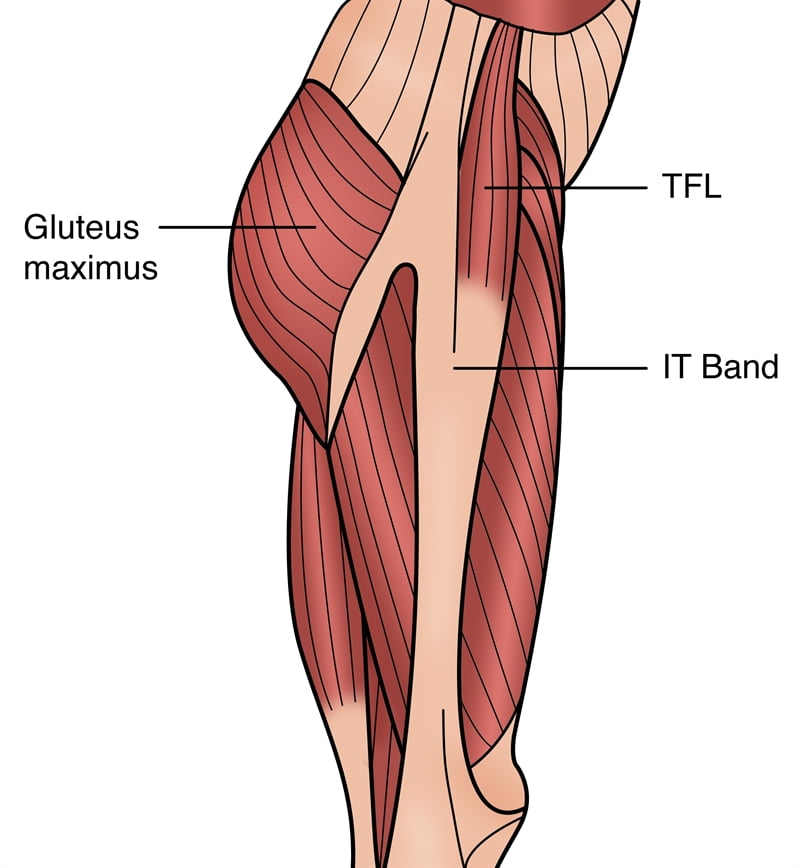
The Tensor Fasciae Latae (TFL) is a small muscle located on the outer side of the hip, playing a crucial role in stabilizing the hip joint and assisting with various movements. Despite its small size, the TFL can cause significant discomfort when it becomes painful or injured. In this article, we will explore the causes, symptoms, and treatments for Tensor Fasciae Latae pain to help you find relief and get back to your active lifestyle.
Contents
What is Tensor Fasciae Latae (TFL)?
Tensor Fasciae Latae (TFL) is a muscle located in the hip region of the body. It is part of the larger group of muscles known as the hip abductors, responsible for moving the leg away from the midline of the body. The TFL is a relatively small, but important muscle that plays a role in stabilizing the hip joint and assisting with various movements, such as walking, running, and climbing stairs.
Also, the TFL originates from the anterior (front) aspect of the iliac crest, which is the upper border of the pelvis, and it inserts into the iliotibial band (ITB), a thick band of connective tissue that runs down the outer side of the thigh to attach to the shin bone (tibia). The TFL and ITB work together to provide stability to the knee and hip during certain movements.
Causes of Tensor Fasciae Latae Pain

Tensor Fasciae Latae (TFL) pain can occur due to various reasons, and it is often associated with the larger issue of iliotibial band syndrome (ITBS). Below are some common causes of TFL pain:
- Iliotibial Band Syndrome (ITBS): ITBS is one of the most prevalent causes of TFL pain. ITBS is an overuse injury by inflammation and irritation of the iliotibial band. It is through a thick band of connective tissue that runs along the outer side of the thigh. When the ITB becomes tight or inflamed, it can cause friction and pain at the insertion point of the TFL, which is near the knee joint.
- Tightness and Overuse: The TFL can become tight and overworked due to repetitive movements, such as running, cycling, or climbing stairs. Activities that involve frequent hip flexion and extension can put a strain on the TFL and contribute to pain.
- Weakness or Muscle Imbalance: Weakness or imbalances in the muscles around the hip and thigh can also lead to TFL pain. If the TFL is overcompensating for weak gluteal muscles, for example, it may become strained and painful.
- Poor Biomechanics: Improper movement patterns or biomechanics during physical activities can contribute to TFL pain. For instance, excessive hip adduction or internal rotation during running or walking can put extra stress on the TFL and ITB.
- Overtraining: Engaging in excessive training or sudden increases in activity level without allowing adequate time for recovery can lead to TFL pain and other overuse injuries.
- Poor Posture: Prolonged periods of sitting or poor posture can cause muscle imbalances and tightness in the hip and thigh region, including the TFL.
Symptoms of Tensor Fasciae Latae Pain
Tensor Fasciae Latae (TFL) pain can manifest with various symptoms, which can vary in intensity and location depending on the underlying cause. The most common symptom associated with TFL pain is:
- Outer Hip Pain: Pain and discomfort are typically felt on the outer side of the hip. The pain may be localized around the TFL muscle or may extend along the iliotibial band (ITB) down the outer thigh toward the knee.
Other symptoms and signs that may accompany TFL pain or be indicative of related conditions (such as iliotibial band syndrome) include:
- Knee Pain: Pain may be felt on the outside of the knee joint due to the insertion point of the iliotibial band near the knee. This is a common symptom of iliotibial band syndrome (ITBS).
- Pain with Activity: TFL pain often worsens with activities that involve repetitive hip movements, such as walking, running, cycling, or climbing stairs. The pain may subside with rest or reduced activity.
- Stiffness: The TFL and surrounding muscles may feel stiff and tight, especially after physical activity or prolonged periods of inactivity.
- Tenderness: The TFL region may be tender to the touch.
- Clicking or Snapping Sensation: Some individuals with TFL pain may experience a clicking or snapping sensation in the hip when moving the leg.
- Weakness: TFL pain and associated conditions can lead to weakness or reduced strength in the hip and thigh region.
- Pain While Crossing Legs: Crossing the legs while sitting may exacerbate TFL pain and discomfort.
- Worsening Pain on Downhill Descents: If iliotibial band syndrome is the underlying cause, pain may worsen when going downhill, as the knee undergoes more flexion during this movement.
Self-Management and Home Remedies

Self-management and home remedies can help manage Tensor Fasciae Latae (TFL) pain and associated conditions like iliotibial band syndrome (ITBS). Here are some strategies you can try:
- Rest: Give your hip and leg a break from activities that exacerbate the pain, such as running or cycling. Adequate rest allows the tissues to heal and reduce inflammation.
- Ice or Heat: Applying ice packs or cold packs to the affected area for 15-20 minutes every few hours can help reduce inflammation and numb the pain. Alternatively, you can use heat packs to relax tight muscles. Apply heat for 15-20 minutes at a time. Always use a barrier like a cloth between your skin and the ice or heat source to avoid skin damage.
- Stretching: Gentle stretching exercises for the hip, including the TFL and ITB, can help improve flexibility and alleviate tension. Perform stretches regularly, holding each stretch for about 30 seconds.
- Strengthening Exercises: Strengthening the muscles around the hip, especially the gluteal muscles, can help provide better support and reduce strain on the TFL. Include exercises like clamshells, hip bridges, and lateral leg lifts in your routine.
- Foam Rolling: Using a foam roller on the outer thigh can help release tension in the TFL and ITB. Roll the foam roller along the outer thigh, focusing on any tender or tight spots. However, avoid rolling directly over bony areas.
- Proper Footwear: Ensure you are wearing appropriate footwear that provides adequate support for your physical activities, especially if you engage in running or other high-impact exercises.
- Modify Activities: Temporarily modify or avoid activities that worsen the pain until you experience significant improvement.
Professional Treatments
If self-management strategies and home remedies do not provide sufficient relief or if the Tensor Fasciae Latae (TFL) pain persists, seeking professional medical treatment is recommended. A healthcare professional, such as a physician or physical therapist, can assess your condition and design a targeted treatment plan based on your specific needs. Here are some professional treatments:
- Physical Therapy: A physical therapist can assess your hip and leg function, identify any muscle imbalances or movement patterns contributing to the TFL pain, and provide tailored exercises and manual therapies to address these issues. They may use techniques like myofascial release, soft tissue mobilization, and stretching exercises to relieve tension in the TFL and surrounding muscles.
- Steroid Injections: In cases of significant pain and inflammation, a physician may administer corticosteroid injections into the TFL region to reduce inflammation and provide temporary relief. However, these injections are usually used sparingly due to potential side effects.
- Extracorporeal Shock Wave Therapy (ESWT): ESWT is a non-invasive procedure that uses shock waves to promote healing and reduce pain in certain musculoskeletal conditions. It may be considered for persistent TFL pain that does not respond to conservative measures.
- Graston Technique or Instrument-Assisted Soft Tissue Mobilization (IASTM): These techniques involve using specialized instruments to massage and mobilize soft tissues, which can be beneficial for relieving TFL tightness and improving mobility.
- Biomechanical Analysis: A healthcare professional may assess your movement patterns, running gait, or sports-specific mechanics to identify any contributing factors to TFL pain. They can then provide recommendations for improving form and reducing stress on the TFL.
Understanding TFL Pain and Hip Anatomy

Understanding the anatomy of the hip and the factors contributing to Tensor Fasciae Latae (TFL) pain can provide valuable insights into how this condition develops. Let’s explore the relevant anatomy:
- Hip Joint: The hip joint is a ball-and-socket joint formed by the head of the femur (thigh bone) fitting into the acetabulum, a cup-shaped socket in the pelvis. It allows for a wide range of movements, including flexion, extension, abduction, adduction, and rotation.
- Tensor Fasciae Latae (TFL) Muscle: The TFL is a small, triangular muscle located on the outer side of the hip. It originates from the anterior (front) part of the iliac crest, the upper border of the pelvis, and inserts into the iliotibial band (ITB). The TFL plays a role in hip flexion and internal rotation and works as one of the hip abductor muscles.
- Iliotibial Band (ITB): The ITB is a thick band of connective tissue that runs along the outer side of the thigh. It originates from the TFL and extends down to attach near the knee, primarily on the lateral epicondyle of the femur. The ITB acts as a lateral stabilizer for the knee and helps maintain hip and knee alignment during activities like walking and running.
- Gluteal Muscles: The gluteal muscles, including the gluteus maximus, gluteus medius, and gluteus minimus, are large in the buttocks that play a significant role in hip extension and abduction. These muscles work in synergy with the TFL to stabilize the pelvis and hip during various movements.
Conclusion
In conclusion, Tensor Fasciae Latae pain can be a debilitating condition that interferes with daily life and physical activities. Understanding the causes, symptoms, and available treatments for TFL pain is essential in finding relief and preventing future discomfort. Implementing self-management techniques, seeking professional care when necessary, and making lifestyle modifications can contribute to improved TFL health and overall well-being.
If you’re experiencing Hip pain, physical therapy for hip pain at PhysioMantra can help: Book an online physical therapy session.